The challenge: Cutaneous T cell lymphoma (CTCL) is a heterogenous disease that presents with a variety of clinical features which involves both the blood and skin. The patients are considered incurable and have limited treatment options with high likelihood of disease relapse. Taken together, this highlights a need for novel and more effective therapies.
The solution: Chimeric antigen receptor (CAR) immune cell therapy is a new pillar of cancer treatment that has demonstrated clear, and enduring, benefits clinically in other blood-based cancer indications. We asked whether a CAR-based approach would deliver a more effective treatment option for CTCL patients.
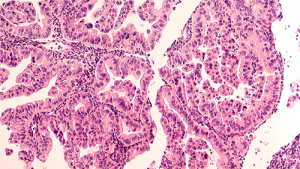
Key outcomes: This study shows for the first time, that tumour-associated glycoprotein-72 (TAG-72) is expressed on disease T cells in CTCL patients and that these cells can be eradicated with TAG-72 targeting CAR-T cells. Our preclinical studies outline that TAG-72 may be a novel target for CAR-T cells therapy for CTCL.
The challenge: Manufacture of chimeric antigen receptor (CAR)-T cells usually involves the use of viral delivery systems to achieve high transgene expression. However, it can be costly and may result in random integration of the CAR into the genome, creating several disadvantages including variation in transgene expression, functional gene silencing and potential oncogenic transformation.
The solution: We optimized the method of nonviral, CRISPR/Cas9 genome editing using large donor DNA delivery, knocked-in an anti-tumor single chain variable fragment (scFv) into the N-terminus of CD3ε and efficiently generated fusion protein (FP) T cells.
Key outcomes: These cells displayed FP integration within the TCR/CD3 complex, lower variability in gene expression compared to CAR-T cells and good cell expansion after transfection. CD3ε FP T cells were predominantly CD8+ effector memory T cells, and exhibited anti-tumor activity in vitro and in vivo. Dual targeting FP T cells were also generated through the incorporation of scFvs into other CD3 subunits and CD28. Compared to viral-based methods, this method serves as an alternative and versatile way of generating T cells with tumor-targeting receptors for cancer immunotherapy.
Published in Frontiers in Immunology (https://doi.org/10.3389/fimmu.2022.968395), Van To and colleagues review the current potential CAR-T cell targets for Cutaneous T cell lymphoma (CTCL), and the strategies required for more effective treatment of the disease. CTCL is a blood cancer caused by malignant T cells. While CAR-T cell therapy has had remarkable success against most types of blood cancers, its application to T cell cancers is limited.
The challenge: CAR-T cell therapies face a range of barriers against T cell cancers. These are associated with the creation and application of the therapy, as well as the cancer cell environment. CAR-T cells are engineered to identify a pre-determined target on cancer T cells. However, since both the malignant T cell and the therapy may share the target, CAR-T cells could kill healthy cells in the patient. Additionally, a shared target may also cause self-killing of the CAR-T cells.
Cancer cells can also reduce their expression of the target, which may lead to therapy resistance, and during the manufacture of CAR-T cells from patient blood, the therapy may become contaminated with cancerous cells.
The solutions: New therapeutic approaches are required as CTCL remains a difficult disease to treat, with low survival in patients, and limited curative options. Approaches to improve therapy barriers include selecting appropriate CAR-T cell targets, ideally with low expression on healthy cells and engineering CAR-T cells with multiple targets using different ‘logic-gate’ strategies tailored to strike the balance between the safety and efficacy of the therapy.
Published in Translational Oncology (https://doi.org/10.1016/j.tranon.2022.101477), Dr Anisha Suraiya and colleagues have demonstrated a novel CAR-T cell carrier system. CAR-T cell therapy aims to target and kill cancer cells, and boost a patient’s immune system to fight cancer. The use of CAR-T cells for the treatment of blood cancers has been revolutionary with unparalleled responses observed in some patients. Despite significant advances, the same positive impact in solid cancers, such as ovarian cancer, remains to be seen.
The challenge: Solid cancers are able to create an environment that supports cancer growth and ‘protects’ cancer cells from elimination. When CAR-T cells are exposed to this complex environment for an extended time their ability to kill cancer cells can be reduced.
The solution: Designing a delivery system that shields CAR-T cells from the impact of the cancer environment may improve outcomes of CAR-T therapy in solid cancers. To this end, Dr Suraiya and colleagues have investigated the use of gelatine-based microgels as CAR-T cell carriers.
Key outcomes: CAR-T cells are able to survive in the microgel carriers for up to seven days. Importantly, encapsulation in microgel carriers did not impact their ability to kill cancer cells. Indeed, CAR-T cells were found to be potent killers of 3D solid tumor cell culture models. This study provides evidence supporting the use of microgel as CAR-T delivery vehicles for the treatment of cancer.
Integrin-linked kinase (ILK) has been implicated as a molecular driver and mediator in both inflammation and tumorigenesis of the colon. However, a role for ILK in the tumor microenvironment (TME) and immune evasion has not been investigated. Here, we show a correlation of ILK expression with the immunosuppressive TME and cancer prognosis. We also uncover a role for ILK in the regulation of programmed death-ligand 1 (PD-L1) expression and immune cell cytotoxicity.
Dr Ian Nisbet Chief Operating Officer
Held in partnership with Harvard Stem Cell Institute, this virtual one-day investor and partner conference will explore stem cell therapeutics in the areas of regenerative medicine, oncology and emerging academic research. It will also showcase cutting-edge science, industry trends and the commercial potential of this innovative sector to an invited group of 65 life science investors.
Company participation in the conference is by invitation only. On Tuesday 12 April at 4:40 am AEST Ian will provide a non-confidential overview of Cartherics, its technology, lead product and pipeline, competitive position and more.
Cartherics Chief Development Officer, Dr Nicholas Boyd
The innate cell therapy field is exploding as novel research charges through the clinic, proving its potential as a safe, efficacious, and cost-effective treatment. From 30 March-1 April 2022 Pacific Daylight Time (PDT) industry experts will meet in San Diego, California to discuss the clinical and phase development of NK, Macrophage, γδT and NKT cell therapies for liquid and solid tumors.
On opening day Nicholas will make a presentation entitled “Optimizing Manufacturing Processes for iPSC-derived Cell Therapy Products”. On Friday PDT he will participate in a panel with representatives from Adicet Bio and Cellularity. They will discuss the complexity of identifying ‘optimal’ donors for off-the-shelf therapies.
Cartherics Chief Development Officer, Dr Nicholas Boyd
CAR-T immunotherapy has exploded over the last half a decade. It is now a billion-dollar market that is expanding rapidly with over 400+ new cell therapy trials in 2021 alone. But challenges still remain in solid tumours, toxicity management and manufacturing innovations. Stakeholders across oncology and beyond are now turning to next-generation developments and technology to create the therapies of tomorrow, NOW!
This week Stakeholders are meeting at the Next Generation CAR-TCR Summit in London, UK. On Friday 25 February at 2:45 am AEDT – in a presentation entitled Allogeneic Solid Tumor Immunotherapy using iPSC-Derived Gene-Edited iNK Cells, Nicholas will discuss why the design, manufacture, delivery and cost of Cartherics’ allogeneic ‘off-the-shelf’ approach is superior to patient-derived allogeneic cell therapies.
Chief Development Officer, Dr Nicholas Boyd
Cell therapies have the potential to not only be life-saving but curative for a host of diseases. However, inherent limitations in autologous based CAR-T therapy face major roadblocks for mass adoption and therapeutic effects in solid tumour indications.
On Friday 28 January at 7:30 am AEDT Nicholas will discuss the design, manufacture and translation of cell therapies in a presentation entitled Advancing Off-The-Shelf Immunotherapy for Solid Tumours: Using Gene-Edited iNK Cells.
Cellular immunotherapy is revolutionizing cancer treatment. And off-the-shelf, or allogeneic, treatments are beginning to replace technologies developed individually for each patient.
This is good news because the potential of allogeneic therapies is great. They promise to significantly save time and cut costs compared to individualised, or autologous, treatments.
In Cells special issue ‘Allogeneic Cell Cancer Immunotherapies” editor Alan Trounson introduces five papers from leading research teams, including two from Cartherics’ scientists. They all tackle the major scientific hurdle the new technologies face: possible rejection of treatments by patients’ immune systems.
Trounson is impressed by the solutions presented. “Early progress is encouraging, but the outcome of human clinical trials remains essential to evaluate the safety and efficacy of these new allogeneic cell therapy approaches,” he notes.
Chief Scientific Officer, Dr Richard Boyd
Deriving “off-the-shelf” cancer fighting immune effector cells from iPSC offers a remarkable opportunity for overcoming the limitations of current autologous CAR-T cell therapies. However as promising as the iPSC approach is, it also presents a series of different challenges.
On 7 December 2021 Richard discussed the challenges and potential solutions. Among the solutions is Cartherics’ platform for creating clinic-ready, gene-edited, CAR-iNK cells for application in solid tumour immunotherapy.
Cellular immunotherapy is revolutionizing cancer treatment. However, autologous transplants are complex, costly, and limited by the number and quality of T cells that can be isolated from and expanded for re-infusion into each patient.
This paper demonstrates a stromal support cell-free in vitro method for the differentiation of T cells from umbilical cord blood hematopoietic stem cells (HSCs).
From autologous cancer killers to off-the-shelf products targeting solid tumours like ovarian, prostate and breast cancer, Cartherics is developing them all.
The potential of such therapies is the reason Cartherics’ Chief Scientific Officer Richard Boyd was invited to speak at the international Multi-Functional Cell Therapies Summit in Boston, 4-6 May 2021.
In his presentation, Richard updated delegates on Cartherics’ recent advances.
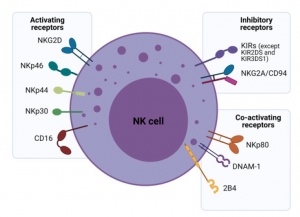
Natural killer (NK) cells are potent innate immune system effector lymphocytes armed with multiple mechanisms for killing cancer cells. Given the dynamic roles of NK cells in tumor surveillance, they are fast becoming a next-generation tool for adoptive immunotherapy. Many strategies are being employed to increase their number and improve their ability to overcome cancer resistance and the immunosuppressive tumor microenvironment.
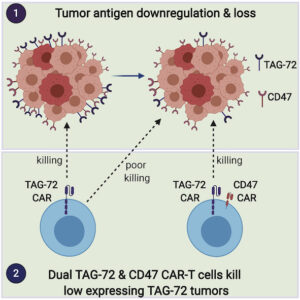
Chimeric antigen receptor (CAR) T cells have revolutionized blood cancer immunotherapy; however, their efficacy against solid tumors has been limited. A common mechanism of tumor escape from single target therapies is downregulation or mutational loss of the nominal epitope.
https://www.cell.com/molecular-therapy-family/oncolytics/fulltext/S2372-7705(21)00002-4
Chimeric antigen receptors (CARs) have been used for efficient destruction of B cell tumors but have been relatively ineffective as therapy for solid tumors. Ovarian cancer is a difficult cancer to treat, with five-year survival rates commonly around 25% of patients at diagnosis.

Off-the-shelf iPSC derived CAR-NK immunotherapy for solid tumors
Principal Scientist Dr Nicholas Boyd
The clinical impact of Chimeric Antigen Receptor T cell (CAR-T) technologies on hematological malignancies have revolutionized cancer treatment.
However, current autologous CAR-T therapies face major roadblocks for mass adoption.
Despite progress in developing cell therapies, such as T cell or stemcell therapies to treat diseases, immunoincompatibility remains a major barrier to clinical application.
Given the fact that a host’s immune system may reject allogeneic transplanted cells, methods have been developed to genetically modify patients’primary cells.
In October 2019 Cartherics attended the prestigious Cell & Gene Meeting on the Mesa https://www.meetingonthemesa.com/ in Carlsbad, California.
Cartherics Chief Scientific Officer, Richard Boyd, presented details to delegates of Cartherics’ pre-clinical in vitro and animal model research, cell manufacture for clinical trials, and corporate game plan.